Why do we use laser for diabetic retinopathy? Part 1 of 2
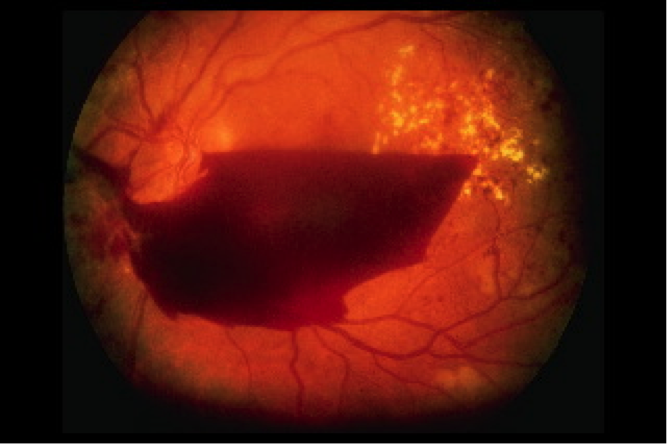
Proliferative Diabetic Retinopathy
Diabetic retinopathy occurs when high levels of blood sugar seen in diabetes mellitus damages the blood vessels of the retina.
The main effects that this can have on the retina are
- oxygen starvation of the retina through damaged blood vessels – this leads to the formation of abnormal blood vessels in the retina, which can bleed – this is known as proliferative diabetic retinopathy
- leakage of fluid in the central part of the retina known as the macula – known as diabetic maculopathy
Laser treatment has been the main treatment for diabetic retinopathy for many years and still remains the main treatment for proliferative diabetic retinopathy today.
So why do we use lasers in the treatment of proliferative diabetic retinopathy?
Well, lasers have the unique ability to target tissue specifically depending on the colour of their wavelength. They can also be fine tuned and adjusted to burn, disrupt or sculpt tissue.
The eye is the perfect organ to use lasers for treatment because it requires a finely focused treatment because of its small size. It also has an open window to the external world – that is how light enters our eye and gets converted to electrical signals that are sent to our brain and interpreted as vision. Laser energy is taken up by the melanin present in the retinal nourishing layer.
So lasers and eyes are very compatible with each other.
The original observation that proliferative diabetic retinopathy did not tend to occur in patients who had peripheral scarring in their retinas from other conditions led researchers to fire lasers at the peripheral retina in patients with proliferative diabetic retinopathy.
This led to peripheral scarring and as a result the abnormal blood vessels that grew in the retina, shrunk and disappeared.
Firing a laser at the peripheral retina and scarring it , does not cause significant loss of vision to patients becausehun the central retina is always spared. The central retina is responsible for the majority of our useful vision such as reading, recognising faces and colour vision. The peripheral retina is responsible for night vision and eccentric viewing.
Sacrificing the peripheral retina to laser burns outweighs the loss of this less useful vision. The result is that the central vision is protected from being lost to a bleed in the eye.
The principle of applying laser retinal burns to the peripheral retina has not changed significantly in the last 40 years. The only real change is the improvement of the technology that allows smaller machines, more focused laser spot delivery and multiple shots applications.
The effectiveness of the peripheral retinal laser or pan retinal photo-coagulation (PRP) has been validated in excellent research studies and it has been shown to be effective in preventing significant vision loss compared to those who do not get treatment.
Does this laser treatment for proliferative diabetic retinopathy hurt?
It can be a uncomfortable for some patients. There are nerve endings near the retina that can cause discomfort. Thankfully our newer multi-shot laser machines can perform this type of laser treatment more quickly and comfortably than before.
I offer the latest laser treatment for proliferative diabetic retinopathy in my private practice. Please feel free to call me on 07919 895 448 and we can discuss in detail what you require if you have concerns.
In my next blog post – read why lasers are used for diabetic maculopathy – a condition that is the leading cause of visual loss in the working age population in the Western World.

![Diabetic Retinopathy – did you know? [Infographic]](https://jaheedkhan.co.uk/wp-content/uploads/2016/05/did-you-know-500x383.jpg)
